Tuberculous meningitis
Pathogenesis I Clinical Features I Diagnostic Features I Complications I Investigations I Treatment I prognosis

Tuberculous meningitis is commonest in children under 5 years of age. Tuberculous meningitis usually arises from the formation of a metastatic caseous lesion in the cerebral cortex or meninges that develops during the lymphohematogenous dissemination of primary infection. This initial lesion increases in size and discharges small numbers of tubercle bacilli into the subarachnoid space. Infrequently, Tuberculous meningitis occurs many years after the infection, when rupture of one or more of the subependymal tubercles discharges tubercle bacilli into the subarachnoid space.
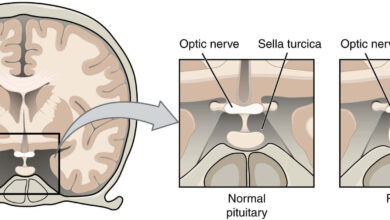
Pathogenesis of Tuberculous Meningitis
Utmost tuberculous infections of the CNS are caused by Mycobacterium tuberculosis. TB bacilli ambit the CNS by hematogenous route secondary to disease elsewhere in the body Tie CNS tuberculosis develops in two stages. Initially small tuberculous lesion (Rich’s foci) develop in the CNS, either during the stage of bacteremia of primary tuberculous infection or shortly afterwards.
These antecedent tuberculous lesions may be in the meninges, the subpial or subependymal exterior of the brain or the spinal cord, and may remain abeyant for years after initial infections. Downstream, rupture or growth of one or more of these small tuberculous lesions produces a buildup of various types of CNS tuberculosis. Breach into the subarachnoid breadth or within the ventricular system results in meningitis.
Intermittently, the infection spreads to the CNS from a site of tuberculous otitis or calvarial osteitis. The pathogenesis of localized brain lesions is also thought to involve hematogenous spread from a primary focus in the lung.
Clinical Features
The signs and symptoms Tuberculous meningitis of progress slowly over several weeks and can be divided into three stages:
1st stage: It typically lasts first 1—2 week. Characterized by non-specific symptoms such as fever, headache, irritability, drowsiness, and malaise. Focal neurological signs are absent.
2nd stage: Usually begin more abruptly. The most common features are lethargy, nuchal rigidity, seizures, positive Kernig or Brudzinski sign, hypertonia, vomiting, cranial nerve palsies, and other focal neurological signs. The stimulating clinical illness usually correlates with the development of hydrocephalus, increased intracranial pressure, and vasculitis. Few children have no evidence of meningeal irritation but may have signs of encephalitis—disorientation, movement disorders, or speech impairment.
3rd stage: Marked by coma, hemiplegia, paraplegia, hyper- tension, decortication, decerebrate posturing, disorientation, deterioration of vital signs, and eventually death.
Is tuberculous meningitis contagious?
The bacteria spread to the brain and spine from another place in the body, usually the lungs. Tuberculous meningitis is very rare in the united states. Most cases are people who travelled to the united states from other countries where Tb is common.
Diagnostic Features
The diagnostic features of Tuberculous meningitis are listed below
- Clinical
- Fever and headache for > 14 days
- Vomiting
- Altered sensorium or focal neurological deficit
- CSF
- Pleocytosis (>20 cells, >500% lymphocytes)
- Increased proteins (> 100 mg/dl)
- Low sugar (<60% of corresponding blood sugar)
- India ink stain (for Cryptococcus) and microscopy for malignant cells should be negative
- Imaging
- Exudates in basal cisterns or in Sylvian fissure
- Hydrocephalus
- Infarcts (basal ganglia)
- Gyral enhancements
- Tuberculoma formation
- Evidence of tuberculosis elsewhere
Complications
Hydrocephalus, cranial nerve palsies, blindness, deafness, hemiplegia or paraplegia, speech impairment, mental retardation, diabetes insipidus, tuberculoma.
Investigations
- CSF analysis:
- Color—hazy/clear/hemorrhagic (rarely).
- Cell count—usually ranges from 10 to 500 cell/mm3
- Polymorphonuclear leukocyte may be present initially, but lymphocytes predominate in the majority of cases.
- CSE glucose—typically <40 mg/dl, but rarely <20 mg/dl.
- CSF proteins—elevated and may be markedly high, 400-500 mg/dl.
- AFB (Acid-fast bacillus) staining and culture. Using conventional Lowenstein Jensen’s medium requires 2-8 weeks to detect the growth of Mycobacterium, while the use of BACTEC 460 TB system requires much less time (1-2 weeks) to isolate T B. CSF ADA (Adenosine deaminase) has a sensitivity of 44-10()% and specificity of 71-100%.
- CBC: Hb%, ESR may be high.
- CXR
- Tuberculin test: 20—50% cases positive. BCG test: 90—100% cases positive
- Gastric aspirates for AFB and culture
- CT/MRI: Thickening and intense enlargement of basilar meninges. Basilar exudate present as intensely enhancing areas in basal cistern governing to spider leg appearance (Pathognomonic for TBM). Hydrocephalus, infarct, ventricular enlargement.
- PCR: To diagnose mycobacterial RNA or DNA sequence in CSF; has a sensitivity of 76% and specificity of 89%.
Treatment
- 2 HRZ/10HR plus Prednisolone 1-2 mg/kg/d in 2 div, doses for weeks and then gradual tapering over 2-4 weeks.
- Fits should be controlled by IV or per rectal diazepam.
- In the acutely ill patient, IV fluid should be restricted to 50ml/kg/d.
Treatment of cerebral oedema, subdural effusion, hydrocephalus and other complications should also be done.
Prognosis
Prognosis is related to the age of the child (young children have a worse prognosis) and the stage of disease at which therapy is commenced. Complete recovery occurs as follows: Stage I 96%, stage II 78%, stage III 21%. 17% of a child in stage III died as opposed to 1% in stage II. Most patients in stage III have permanent disabilities including blindness, deafness, paraplegia, diabetes insipidus, or mental retardation.