Surgery
Gas gangrene
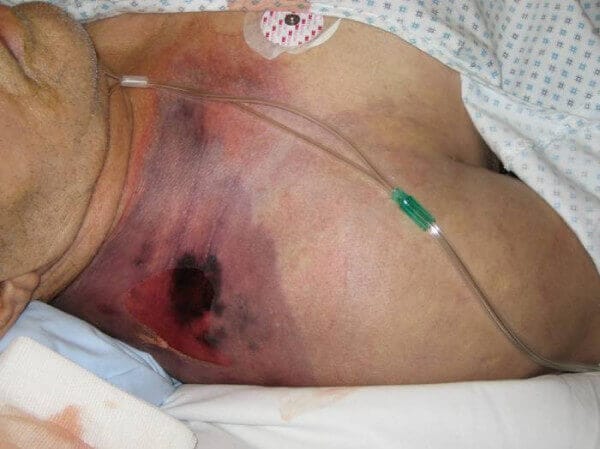
Gas gangrene is infective gangrene caused by clostridial organisms involving mainly skeletal muscle as oedematous myonecrosis. Earlier it was called malignant edema.
Source and Predisposing Factors
- Contaminated, manured or cultivated soil, intestines are the sources. Faecal flora commonly contains clostridial organisms enters the wound; in the presence of calcium from a blood clot or silica (silicic acid) of soil, it causes infection.
- It is common in crush wounds, following road traffic accidents, after amputations, ischaemic limb, gunshot wounds, war wounds. Injury or ischaemia or necrosis of the muscle due to trauma predisposes infection.
- Anaerobic environments in the wound—initial infection with aerobic organism utilises existing oxygen in tissues creating an anaerobic environment to cause clostridial sepsis.
Organisms
- Clostridium Welchii (Perfringens): Gram-positive, anaerobic central spore-bearing, nonmotile, capsulated organisms, most common—60%.
- Clostridium Oedematiens.
- Clostridium septicum.
- Clostridium histolyticum.
Various strains include—A, B, C, D, E.
‘A’ strain is most common.
NOTE: Non-clostridial gas-producing organisms like coliforms can also cause gas gangrene.
Clostridium Welchii produce toxins
• Alpha (most common) • Beta • Epsilon • Iota • Phi toxin – myocardial depressant • Kappa toxin – the destruction of connective tissue and blood vessels • Bursting factor and circulating factor
Exotoxins
- Lecithinase is important toxin which is haemolytic, membranolytic and necrotic causing extensive myositis. It splits lecithin into phosphocholine.
- Haemolysin causes extensive haemolysis.
- Hyaluronidase helps in the rapid expanse of gas gangrene.
- Proteinase causes breaking down of proteins in infected tissue.
Spores enter through the devitalised tissues commonly
in road traffic accidents, crush injury
↓
Spores germinate
↓
Released bacteria will multiply
↓
Exotoxins are released to cause their effects
Effects
- Boundless necrosis of muscle production of gas (hydrogen sulphide; nitrogen; carbon dioxide)which stains the muscle brown or black anaerobic myositis/myonecrosis.
- Usually, muscle is concerned from origin to insertion.
- Often may aggrandize into thoracic and abdominal muscles.
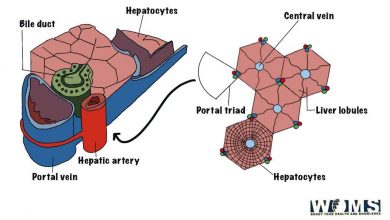
- When it aspires the liver it causes necrosis with frothy blood-foaming liver, is characteristic.
- expeditiously spreading infection which is also often fatal.
- Limbs are generally involved, but organs like liver can also be affected.
- Muscle glycogen is broken down into lactic acid, CO2 and hydrogen. Proteinase liberated by organism forms amino acids which further releases ammonia and hydrogen sulphide. The acid released earlier is neutralised by ammonia and calcium to progress further multiplication of organisms.
Clinical Features
- The incubation period is 1-2 days.
- Features of toxaemia, fever, tachycardia (out of proportion to fever) pallor.
- The wound is under tension with abhorrent smelling discharge (sickly Sweety/ decaying apple odour).
- Khaki brown coloured skin due to haemolysis.
- Crepitus can be felt.
- Jaundice may be an ominous sign and also oliguria signifies renal failure.
- Frequent sites are adductor region of the lower limb and buttocks and subscapular region in the upper limb.
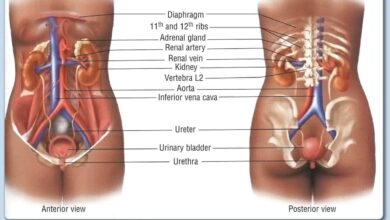
Clostridium Welchii can contaminate limbs, abdominal wall, appendix, gallbladder, common bile duct, intestine, uterus (during septic abortion).
Clinical Types
- Fulminant type causes rapid progress and often death due to toxaemia, renal failure or liver failure or MODS or ARDS.
- Enormous type involving the whole of one limb containing fully dark coloured gas-filled areas.
- Group type: Infection of one cartel of muscles, extensors of the thigh, flexors of the leg.
- Single muscle type affecting one single muscle.
- Subcutaneous type of gas Gangreneimplicateonly subcutaneous tissue (i.e. superficial involvement). It is mainly of anaerobic cellulitis type without muscle involvement usually caused by less virulent clostridial organisms other than clostridial Welchii. It is usually superficial but may spread and involve fascial planes. It causes necrosis with foul-smelling seropurulent discharge
Complications of gas gangrene
- Septicaemia,toxaemia.
- Renal failure, liver failure.
- Circulatory failure, DIC, secondary infection.
- Death occurs in critically ill patients.
Investigations
- X-ray demonstrates gas in muscle plane or under the skin.
- Liver function tests, blood urea, serum creatinine, total count, P02, PCO2.
- CT scan of the part may be useful especially in the chest or abdominal wounds.
- Gram stain shows Gram-positive bacilli.
- Robertson ‘s cooked meat media is used which causes the meat to turn pink with the sour smell and acid reaction.
- Clostridium Welchii is mature in culture media containing 20% human serum in a plate. Antitoxin is placed in one-half of the bacteria grown plate sparing the other half. Zone of opacity will be seen in that half of the plate where there is no antitoxin. In the other half part of the plate where there is antitoxin, there is no opacity—Nagler reaction.
Prevention of gas gangrene
- Proper debridement of devitalised crushed wounds
- Devitalised wounds should not be sutured
- Adequate cleaning of the wounds with H2O2 and normal saline
- Penicillin as a prophylactic antibiotic.
Treatment
- Injection benzylpenicillin 20 lacs 4th hourly + Injection metronidazole 500 mg 8th hourly + Injection aminoglycosides (if blood urea is normal) or third-generation cephalosporins or metronidazole.
- Fresh blood transfusion.
- Polyvalent antiserum 25,000 units injected intravenously after a test dose and repeated after 6 hours (Welchii 10,000 IU, oedematiens 10,000 IU, and septicum 5,000 IU).
- Hyperbaric oxygen is very useful. Liberal incisions are given. All dead tissues are excised and debridement is done until healthy tissue bleeds.
- Rehydration and care optimum urine output (30 ml/hour) (0.5 ml/kg/hour).
- Electrolyte management.
- In severe cases amputation has to be done as a life-saving procedure—stump should never be closed (Guillotine amputation).
- Often ventilator support is required.
- Once award or operation theatre is used for a patient with gas gangrene, it should be fumigated for 24-48 hours properly to prevent the risk of spread of infection to other patients, especially with open wounds.
- Hypotension in gas gangrene is handled with whole blood transfusion.
- Therapy should be concentrated in managing dehydration, hypotension, infection, toxaemia by hydration, fresh whole blood transfusion, passive immunisation, antibiotics, and hyperbaric oxygen, doing radical wound excision with removal of all departed tissues with foreign body or amputation with critical care.