What are the causes of Hives (Urticaria)
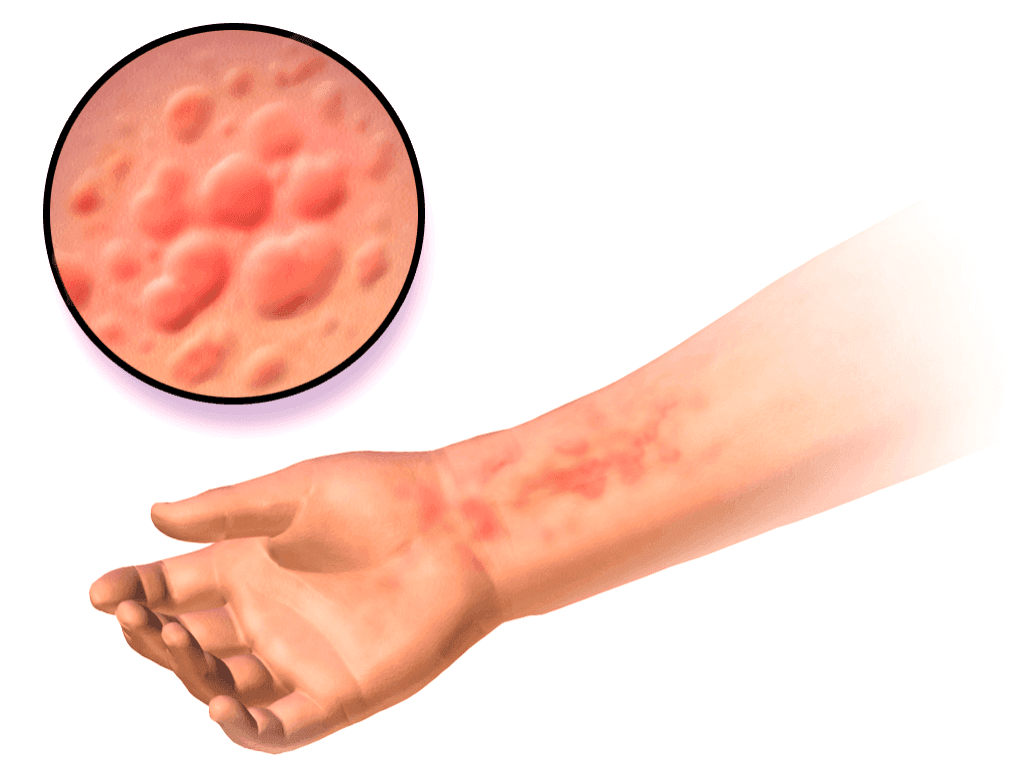
Urticaria also known as hives, is an outbreak of bulgy pale red bumps on your skin that appear abruptly – either as result of the body reaction to allergens or due to some unknown reasons. it is also called welts or wheals, on the skin. The common causes of hives or urticaria are a reaction to allergens.
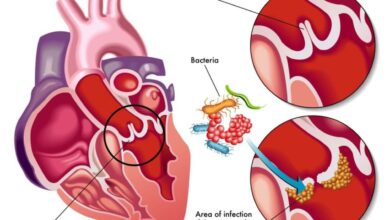
Hives are caused by localised dermal oedema secondary to an interim increase in capillary permeability. If oedema implies subcutaneous or submucosal layers, the terminology angioedema is used.
Urticaria usually causes itching, but may also burn on sitting. The main causes of hives (urticaria) are discussed in the principal article.
Clinical features
Acute urticaria may be associated with angioedema of the lips, face, tongue, throat and rarely, wheezing, abdominal pain, headaches and even anaphylaxis. Urticaria presents for less than 6 weeks is considered to be acute, and chronic if it continues for more than 6 weeks.
Individual weals (definition: evanescent discrete areas of dermal oedema, often centrally white due to masking of local blood supply by a fluid; weals can papules, macules, patches and plaque, last for less than 243 hours.
If they persist, urticaria vasculitis needs to be considered. Clarification of the duration of urticaria can be achieved by drawing around the weal and re-assessing 24 hours later.
History-taking should be a probe for possible causes of hives (Urticaria), including medication. Physical triggers can also be assessed in challenge testing, such as eliciting demographic or pressure testing.
Enquiry about family history and medication, particularly ACE inhibitors, is important in angioedema. The examination may be unremarkable or weals may be evident. The skin should be stroked firmly with an orange stick in order to ascertain whether demographic is present or not.
Mast cell degranulation and release of histamine and other vasoactive mediators is the basis of urticaria. ‘Chronic idiopathic’ or ‘chronic ordinary’ urticaria) is the most common chronic urticaria and has autoimmune pathogenesis in some cases.
Common Causes of hives (Urticaria)
Urticaria occurs when the body reacts to allergens and release histamines and other chemicals from under the surface of the skin. So in short the common causes of hives is the reaction to allergens.
Acute and chronic urticaria
- Autoimmune: due to antibodies that cross-link the IgE receptor on mast cells
- Allergens in foods and inhalants
- Contact allergens: latex, animal saliva
- Drugs
- Physical stimuli: heat, cold, pressure, sun, sweat, water
- Infections: intestinal parasites, hepatitis
- Others: SLE (systemic lupus erythematosus), pregnancy, thyroid disease
- Idiopathic: chronic spontaneous urticaria and angioedema
Urticarial vasulitis
- Hepatitis B, SLE, Idopathic
Investigations
- Investigations should be guided by the history and possible causes of hives but are often negative, particularly in acute urticaria. Some or all of the following may be appropriate:
- Full blood count: eosinophilia in parasitic infection or drug cause.
- Erythrocyte sedimentation rate (ESR) or plasma viscosity: elevated in vasculitis.
- Urea and electrolytes, thyroid and liver function test, iron studies: may reveal an underlying systemic disorder.
- Total IgE and specific IgE to possible allergens: Shellfish, peanut, house-dust mite. Particularly relevant if there is angioedema.
- Autoantibodies, particularly antinuclear factor: positive in systemic lupus erythematosus (SLE) and often positive in Urticarial Vasculitis. Other autoimmune diseases such as Rheumatoid arthritis and autoimmune hepatitis or thyroid disease, may be associated.
- Complement C₃ and C₄ levels: if these are low due to complement consumption, C₁ esterase inhibitor activity should be measured.
- Infection screen: hepatitis screen and HIV may be indicated
- Skin biopsy: if urticaria vasculitis is suspected.
- Challenge tests: to conform to physcial urticarias, such as dermographism, pressure, heat, cold.
Management
Removal or treatment of any trigger is essential, although this may not be identified in the majority of cases. Urticaria may be precipitated by aspirin, NSAIDs, codeine and Opioids, and it is advisable to suggest alternatives such as paracetamol. In chronic Urticaria, non-sedating antihistamines, such as fexofenadine, loratadine or cetirizine, are usually beneficial.
If there is a lack of response after 2 weeks, an alternative non-sedating antihistamine should be used and H₂-blocker, such as cimetidine or ranitidine, can be added. Mast cell stabilisers or leukotriene receptor antagonist, such as montelukast, can be used for more recalcitrant disease. For chronic Urticaria, narrowband UVB phototherapy is valuable and has proven efficacy.
Systemic glucocorticoids are widely prescribed for urticaria but are not indicated in the majority of cases. If systemic glucocorticoids are used, efficacy may be seen only at relatively high doses and they re-appropriate only for occasional short courses in the acute setting, usually in association with angioedema.
Patients with a history of life-threatening anaphylaxis, as in peanut or wasp sting allergy, should carry self-administered adrenaline (epinephrine) injections kit. The IgE monoclonal antibody omalizumab may be effective in patients with severe recalcitrants urticaria.
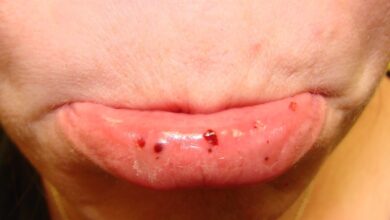
Hives on face
The causes of hives on the face may be allergens in foods and drink, drugs, physical stimuli like heat, cold, sun pressure, sweats, water and more. It can be also caused by infections like intestinal, parasite and hepatitis. Some pictures of hives on the face are:
Hives caused by stress
One cause of hives (urticaria) or factors that makes hives symptoms worse is emotional stress. A study a few years back linked stressful life events, low family supports, broken heart, insomnia, and hives in 75 per cent.
Other scientists have explained how “chronic stress can lead to dysregulation of the mediators and exacerbates underlying inflammatory disease pathophysiology.”
In other words, when a person is fully stressed, any inflammatory reactions are likely to be more astringent in a person who is susceptible to a reaction. This is the way in which hives are caused by stress.
In conclusion
Urticaria is a red, raised, an itchy skin rash that is sometimes triggered by an allergen. An allergen is something that produces allergic reactions. Urticaria is also known as hives, welts, weals, or nettle rash.
Hives affect 20% of people at some time in their life. It is not contagious. The causes of hives are discussed above. If you have any question regarding urticaria, do comment below in the comment box.